Over time, the protective cartilage lining the joints can deteriorate, leading to bone-on-bone friction that limits basic physical actions and causes pain. Hip pain changes the way you navigate daily activities and affects your overall mobility. For individuals facing persistent discomfort, a hip replacement operation provides a viable path to restoring movement.
What Is a Hip Replacement?
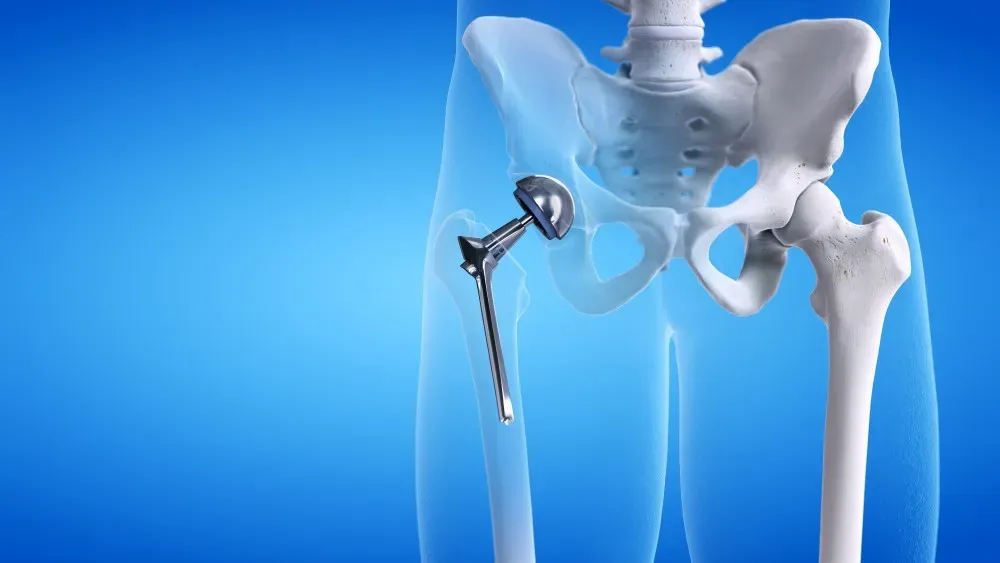
A hip replacement surgery involves removing damaged bone and cartilage from the joint, then substituting them with prosthetic components. Surgeons use artificial parts made from metal, ceramic, or highly durable plastics to replicate a healthy joint. The primary goal centers on pain reduction and function restoration for the patient. During a total joint operation, the specialist replaces the head of the femur with a prosthetic stem and ball. The surgeon then resurfaces the pelvic socket and inserts a metallic cup lined with a smooth spacer. This resulting artificial joint functions much like the original anatomical structure.
Who Benefits From One?
Joint degeneration manifests through specific physical signs that disrupt standard functioning. The primary symptom leading to this surgical intervention involves persistent pain, typically radiating through the hip or groin area. This pain often persists during rest and intensifies with weight-bearing activities. Patients also experience noticeable stiffness in the hip joint, which limits their range of motion and makes lifting the leg exceedingly difficult.
Conditions such as osteoarthritis, rheumatoid arthritis, and osteonecrosis serve as the typical underlying causes for these symptoms. Osteoarthritis wears away the protective cartilage over decades, while rheumatoid arthritis triggers an immune response that causes inflammation and joint erosion. When conservative treatments no longer provide relief, surgical intervention becomes the next logical step.
How Can You Prepare?
Proper preparation facilitates a smoother surgical experience and aids in the recovery process. Prior to the scheduled date, your medical team can conduct a thorough preoperative evaluation. This assessment may include blood tests and a comprehensive review of your current medications. You must discuss all supplements and prescriptions with your doctor, as you might need to stop taking certain medications leading up to the procedure.
Preparing your home environment stands as a necessary step for postoperative safety. Remove tripping hazards such as loose carpet and electrical cords from your main walking paths. Install grab bars in the bathroom and acquire a raised toilet seat. You will need a clear, flat pathway to navigate your house using a walker or crutches. Arrange for a friend, family member, or professional caregiver to assist you with daily tasks, like cooking, bathing, and cleaning, during the first few weeks of recovery.
Confer With a Joint Specialist
While preparing for the physical aspects of recovery requires diligence, understanding the long-term maintenance of your prosthetic joint dictates the overall success of the procedure. You will need to schedule periodic follow-up appointments and X-rays with your orthopedic provider over the years to monitor the alignment and integrity of the implant. Discuss these long-term care strategies with an orthopedic surgeon. They can help determine the best approach for your specific medical history and lifestyle requirements.